The Silent Fire Inside You: How Chronic Inflammation Is Quietly Feeding Your Cancer Risk
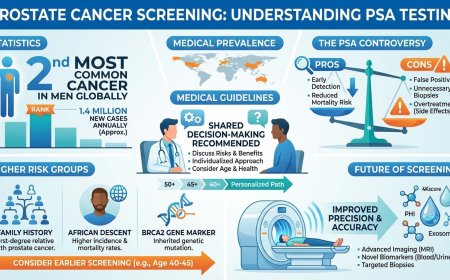
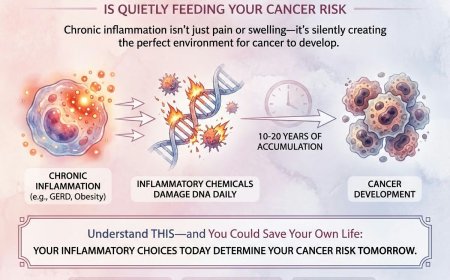
Chronic inflammation isn't just pain or swelling—it's silently creating the perfect environment for cancer to develop. Up to 25% of all cancers are directly linked to long-term inflammation from conditions like GERD, ulcerative colitis, hepatitis, and obesity. While you're ignoring that persistent heartburn or joint pain, inflammatory chemicals are damaging your DNA daily, accumulating mutations over 10-20 years until cancer appears. This comprehensive guide reveals the terrifying inflammation-cancer connection, explains what's happening inside your cells right now, shares real patient stories, and provides actionable steps to control inflammation before it's too late. Your inflammatory choices today determine your cancer risk tomorrow.

At A Glance
You've had that nagging joint pain for years. That persistent acid reflux. The skin condition that never quite goes away. The doctor called it "chronic inflammation" and gave you pills. You took them sometimes. Forgot most days. Because inflammation sounds harmless. It's just swelling, right?
Wrong.
Inside your body right now, chronic inflammation is doing something far more sinister than causing pain or discomfort. It's creating the perfect environment for cancer cells to develop, grow, and spread. Every day you ignore it, you're quite literally feeding potential tumors. This article reveals the connection between inflammation and cancer that deserves your full attention — what's happening in your cells right now, and why controlling inflammation today could prevent cancer tomorrow.
The Fire You Can't See (But Should Fear)
Think of inflammation like this:
Acute inflammation = A firefighter putting out a house fire. Quick response. Does the job. Leaves when finished.
Chronic inflammation = That same fire smoldering in your walls for years. Never fully extinguished. Slowly weakening the entire structure. Eventually, the whole building collapses.
Here's what you need to understand:
When you cut your finger or catch a cold, inflammation is your friend. It rushes healing cells to the site, fights infection, repairs damage. This acute inflammation lasts days or weeks, then disappears.
But chronic inflammation? That's a different beast entirely.
It's inflammation that never shuts off. It runs continuously for months, years, even decades. And while it's burning slowly inside you, it's doing something most people never realize:
It's creating the ideal conditions for cancer to develop.
The Inflammation-Cancer Connection Your Doctor Didn't Explain
Here's the scientific reality:
Up to 25% of all cancers are directly linked to chronic inflammation.
One in four cancers develops because of long-term inflammation in the body.
Specific examples:
Chronic hepatitis (liver inflammation) → Liver cancer Ulcerative colitis/Crohn's disease (intestinal inflammation) → Colorectal cancer Chronic pancreatitis (pancreas inflammation) → Pancreatic cancer H. pylori infection (stomach inflammation) → Gastric cancer Chronic acid reflux/GERD (esophageal inflammation) → Esophageal cancer Chronic bronchitis (lung inflammation) → Lung cancer
Notice the pattern? Chronic inflammation in an organ significantly increases cancer risk in that exact organ.
But here's what makes this particularly concerning:
Most people with chronic inflammation have no idea they're at increased cancer risk.
What's Happening Inside Your Body Right Now
Let's walk through the cellular process of chronic inflammation:
Stage 1: The Initial Insult (You barely notice)
Something triggers inflammation in your body:
Poor diet (high sugar, processed foods, trans fats), chronic infection (H. pylori, hepatitis, HPV), obesity (fat cells release inflammatory chemicals), smoking (constant lung tissue damage), chronic stress (cortisol disruption), and autoimmune conditions.
Your immune system activates. Sends inflammatory cells to the area. This is supposed to be temporary.
But for many people, it never stops.
Stage 2: The Persistent Fire (You feel "off")
Months pass. Years pass. The inflammation continues.
Your immune cells release chemicals including cytokines (inflammatory messengers), reactive oxygen species (free radicals that damage DNA), and growth factors (signals that tell cells to multiply).
You may feel fatigue that never quite goes away, joint pain you've accepted as "getting older," digestive issues you manage with antacids, and unexplained weight gain.
You think: "This is just life now."
Your cells are under constant biochemical stress.
Stage 3: The DNA Damage Accumulates (You have no symptoms)
Here's where cancer begins:
Those inflammatory chemicals attack your DNA every single day.
Normally, your cells repair DNA damage quickly. But chronic inflammation overwhelms your repair systems.
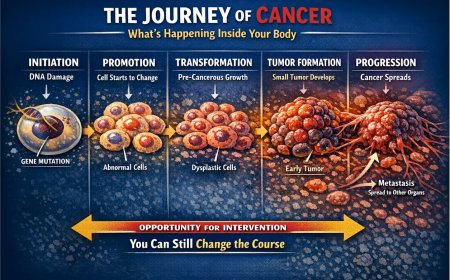
Small mutations accumulate over time. The first mutation may cause a cell to ignore normal growth signals. A second mutation may cause slightly faster cell division. A third may cause the cell to ignore stop signals. A fourth may allow the cell to evade immune detection. A fifth may result in a cancerous cell.
This process takes years — often 10 to 20 years.
Which means the chronic inflammation you're ignoring today could manifest as cancer a decade or more from now.
Stage 4: The Cancer-Friendly Environment (Still no obvious symptoms)
Even if cells haven't turned cancerous yet, chronic inflammation creates conditions in which cancer can thrive. It promotes blood vessel growth that can feed tumors, suppresses normal immune surveillance, increases cell multiplication (creating more opportunities for mutations), prevents damaged cells from dying, and breaks down tissue barriers that would otherwise limit cancer spread.
Stage 5: The Diagnosis (Symptoms finally appear)
Ten years later. Fifteen years later. Twenty years later.
You feel a lump. See blood in your stool. Develop a persistent cough. Lose weight unexpectedly.
The doctor orders tests.
"I'm sorry. It's cancer."
And you think: "How did this happen? I thought I was just dealing with my chronic heartburn / colitis / hepatitis / joint pain."
Now you know how it happened.
The inflammation you ignored for years finally completed its work.
Real Stories That Should Move You to Action
Story #1: Ramesh, 52, Mumbai
The Background: Chronic heartburn for 15 years. Took antacids daily. Never investigated the root cause. Assumed it was "just stress" from work.
The Reality: His chronic acid reflux caused Barrett's esophagus — a precancerous condition where stomach acid repeatedly damages esophageal tissue, causing chronic inflammation and cellular changes.
The Diagnosis: At 52, difficulty swallowing and weight loss led to an endoscopy that revealed Stage 3 esophageal adenocarcinoma.
The Treatment: Esophagectomy (surgical removal of the esophagus), with a portion of the stomach repositioned into the chest, followed by six months of chemotherapy and radiation, resulting in permanent difficulty eating and significant weight loss.
His Words: "For 15 years, I knew something was wrong. I felt that burning every single day. I just kept taking antacids and ignoring it. If I'd gotten an endoscopy at year 2 instead of year 15, they would have caught the Barrett's early. They could have monitored it. Maybe prevented the cancer entirely."
Story #2: Anjali, 38, Bangalore
The Background: Diagnosed with ulcerative colitis at age 25. Moderate to severe inflammation in her colon. Took medications inconsistently. "It didn't bother me that much. Only flared up sometimes."
The Reality: Every single flare-up was causing more DNA damage in her colon cells. Every time she skipped medication, inflammation persisted unchecked.
The Diagnosis: At 38, a colonoscopy (which she had delayed) revealed Stage 2B colon cancer.
The Treatment: Partial colectomy, temporary colostomy, chemotherapy, and reversal surgery.
Her Words: "They told me at diagnosis that ulcerative colitis increases colon cancer risk. I heard them. But I was 25. Cancer felt like something that happened to other people. Older people. I didn't connect my daily inflammation to future cancer. Thirteen years of uncontrolled inflammation created my tumor. It didn't have to be this way."
The Five Dangerous Myths About Inflammation
Myth #1: "Inflammation just means swelling and pain"
The Reality: Inflammation is a complex immune response involving dozens of chemical messengers, immune cells, and molecular changes. The swelling and pain you feel are just the surface symptoms. The real damage — DNA mutations, cellular dysfunction, tissue remodeling — happens silently at the molecular level.
You can have severe chronic inflammation with minimal or no pain.
Myth #2: "Taking anti-inflammatory pills occasionally is enough"
The Reality: Taking an ibuprofen or aspirin occasionally doesn't address chronic inflammation. These medications provide temporary symptom relief but don't eliminate the underlying cause.
If you have chronic inflammation from obesity, you need to address weight. If from poor diet, you need to change eating habits. If from chronic infection, you need to eradicate the infection. If from autoimmune disease, you need proper disease management.
Symptomatic medication alone is not sufficient to reduce cancer risk.
Myth #3: "I don't have inflammation because I don't have any symptoms"
The Reality: Some of the most dangerous inflammation is completely silent.
Blood tests showing elevated C-reactive protein (CRP), erythrocyte sedimentation rate (ESR), or interleukin-6 (IL-6) indicate systemic inflammation even in people who feel perfectly fine.
You could have chronic liver inflammation (hepatitis), chronic stomach inflammation from H. pylori, or chronic low-grade systemic inflammation from obesity — all without noticeable symptoms — until more serious disease develops.
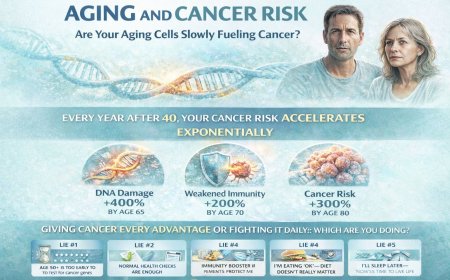
Myth #4: "Inflammation is just a natural part of aging"
The Reality: While some increase in inflammatory markers occurs with age, high levels of chronic inflammation are not normal and should not be accepted.
This concept — called "inflammaging" — is increasingly recognized as a disease process, not an inevitable natural state. Research consistently shows that people who control inflammation through lifestyle measures live longer, have lower cancer rates, maintain better cognitive function, and experience less chronic disease overall.
Inflammation is manageable — not an inevitability.
Myth #5: "My inflammation is under control because I take my prescribed medication"
The Reality: Medications help, but they are often not sufficient alone.
Research in inflammatory bowel disease shows that patients who combine medication with lifestyle changes — including diet improvement, stress management, and adequate sleep — achieve meaningfully better disease control, fewer flare-ups, and lower inflammatory markers compared to those on medication alone.
If you're taking medication but still consuming inflammatory foods, living with chronic stress, sleeping fewer than six hours a night, or carrying significant excess weight, your inflammation may not be fully controlled.
The Inflammation-Cancer Triggers Hiding in Your Daily Life
Dietary Triggers (Feeding the Fire Daily)
High-risk foods include processed meats such as salami, hot dogs, and bacon, which contain nitrates that can trigger inflammatory responses. Refined carbohydrates like white bread and pastries cause blood sugar spikes that provoke inflammation. Trans fats found in fried and heavily processed foods directly activate inflammatory pathways. Excessive alcohol causes liver inflammation, which increases cancer risk. High-sugar foods create oxidative stress and contribute to chronic inflammation.
Research has linked daily consumption of processed meat to meaningfully higher colorectal cancer risk, partly through the mechanism of chronic intestinal inflammation from nitrates and preservatives.
Lifestyle Triggers (The Silent Accelerators)
Obesity: Fat tissue is not metabolically inert. It actively releases inflammatory chemicals including TNF-alpha, IL-6, and C-reactive protein. Individuals with significant excess weight carry chronic systemic inflammation even without any other diagnosed condition. This inflammation is associated with increased risk of breast cancer (post-menopausal), colon cancer, esophageal cancer, kidney cancer, pancreatic cancer, and liver cancer.
Chronic Stress: Sustained stress keeps cortisol elevated, which disrupts immune function, increases inflammatory markers, impairs DNA repair mechanisms, and creates oxidative stress. Research suggests chronic psychological stress is associated with a measurable increase in cancer risk across several cancer types.
Poor Sleep: Consistently sleeping fewer than six hours per night is associated with elevated CRP, increased IL-6, impaired immune surveillance, and greater DNA damage accumulation over time.
Infection Triggers (The Invisible Invaders)
H. pylori infects approximately half the global population, causes chronic gastritis, and is associated with a significantly elevated risk of gastric cancer. Eradication of H. pylori infection has been shown to reduce this risk substantially.
Hepatitis B and C cause chronic liver inflammation and are associated with dramatically increased liver cancer risk. The majority of hepatocellular carcinoma (liver cancer) cases globally are linked to chronic viral hepatitis.
HPV (human papillomavirus) causes chronic cervical inflammation and is present in the vast majority of cervical cancers. Vaccination against HPV prevents the infections that drive this inflammatory process and substantially reduces cervical cancer risk.
The Testing You Need (And Keep Postponing)
Stop guessing. Start knowing. Here's what to discuss with your doctor:
Blood Tests for Inflammation:
C-Reactive Protein (CRP) is a standard marker of systemic inflammation. A normal result is generally below 1 mg/L; results between 1 and 10 mg/L suggest moderate inflammation; results above 10 mg/L indicate significant inflammation requiring investigation. Erythrocyte Sedimentation Rate (ESR) is another indicator of systemic inflammation and, when combined with CRP, gives a clearer overall picture. A Complete Blood Count (CBC) can reflect chronic inflammation patterns as well.
If your results are elevated, work with your doctor to determine the cause.
Specific Condition Testing:
If you have chronic heartburn or GERD lasting more than five years, discuss an upper endoscopy with your doctor. This procedure can detect Barrett's esophagus and precancerous changes that are entirely treatable when caught early.
If you have inflammatory bowel disease, colonoscopy surveillance — typically every one to two years after eight years of disease — is standard of care and can detect precancerous changes before they progress.
If you have chronic hepatitis, regular liver function tests, viral load monitoring, and liver ultrasound are part of standard surveillance. Your hepatologist will advise on the appropriate schedule.
If you are obese without a known inflammatory diagnosis, a comprehensive metabolic panel and inflammatory markers can establish your baseline and track improvements with weight management.
What You Must Do in the Next 7 Days
Days 1–2: Assessment
Document your inflammation status. Do you have diagnosed inflammatory conditions? Do you have chronic symptoms such as heartburn, joint pain, digestive problems, or skin conditions? Is there a family history of inflammatory conditions or related cancers? Write everything down.
Book an appointment with your general practitioner and request CRP, ESR, and CBC at minimum. Request condition-specific tests if you have known inflammatory diagnoses. Do not delay this.
Days 3–4: Specialist Consultation (If Needed)
If you have chronic GERD lasting more than five years, seek a gastroenterologist. If you have IBD, Crohn's disease, or ulcerative colitis, a gastroenterologist is your key specialist. If you have chronic hepatitis, a hepatologist should be involved. If you have chronic pancreatitis, a gastroenterologist is appropriate. If you have autoimmune conditions, a rheumatologist should be part of your care team.
Book screening procedures as appropriate. Endoscopy if you have chronic GERD. Colonoscopy if you have IBD. These procedures exist precisely to catch problems before they become cancers.
Days 5–7: Immediate Lifestyle Changes
Start today — don't wait for test results.
Adopt an anti-inflammatory dietary approach: eliminate processed meats, reduce red meat to once or twice weekly, increase fatty fish (rich in omega-3s) two to three times weekly, add turmeric, ginger, and garlic to daily cooking, eat five or more servings of vegetables per day, and choose whole grains over refined carbohydrates.
If you carry excess weight, even a five to ten percent reduction in body weight produces measurable reductions in inflammatory markers. Begin with daily walking and honest caloric awareness.
Prioritize sleep. Seven to eight hours of consistent, quality sleep is not optional — it is a biological necessity with documented effects on inflammation and immune function.
Manage stress actively. Ten minutes of daily breathing or meditation, regular physical activity, and professional support where needed all reduce chronic stress and, with it, inflammatory burden.
Professional Support Options
If you're experiencing possible cancer symptoms, seeking a second opinion, or unsure which tests or treatments are right for you, don't wait. Speak with a qualified specialist today.
Connect with experienced U.S.-based cancer specialists for a comprehensive second-opinion consultation. They will carefully review your case and help determine the most appropriate next steps for your individual health needs:
👉 https://myamericandoctor.com/our-doctors/
You may also choose to enroll in our upcoming concierge medical clinic in India, Global Concierge Doctors. We offer U.S.-style primary care with 24/7 access to India-based physicians for ongoing guidance on any health concern. When required, we coordinate referrals to trusted specialists in India and the U.S. for advanced evaluation and care.
Your health decisions today shape your life tomorrow.
The Final Word: Your Body's Message to You
If your chronically inflamed tissue could speak, here's what it would say:
"I've been sending signals for years. Pain. Discomfort. Fatigue. You ignored them all."
"You called it 'just heartburn.' 'Just stress.' 'Just getting older.'"
"But I'm not 'just' anything. I'm chronic inflammation. And I'm methodically creating the conditions for cancer to develop."
"Every day you ignore me, I damage more DNA. Create more mutations. Build more cancer-friendly environments."
"You have a choice. Control me, or I'll eventually control you."
"When I finally succeed in creating cancer, you'll say: 'How did this happen?'"
"And I'll say: 'I told you. For years. You just weren't listening.'"
Take Action Now
Step 1: Book a doctor appointment for inflammatory marker testing. Step 2: Schedule a screening procedure if you have a chronic inflammatory condition. Step 3: Eliminate one inflammatory food from your diet today. Step 4: Tell someone close about your inflammation concerns — accountability matters. Step 5: Set a phone reminder to take anti-inflammatory medications (if prescribed) every single day.
Your inflammation is talking. Are you finally ready to listen?
Reader Poll
Do you have chronic inflammation you've been ignoring?
[ ] Yes, and I'm getting tested this week [ ] Yes, but I've been avoiding getting checked [ ] I'm managing my inflammation actively [ ] I don't think I have inflammation
Share This Article
Know someone with chronic heartburn who "just takes antacids"? Know someone with inflammatory bowel disease who skips medications? Know someone carrying significant excess weight who dismisses inflammation as "just being heavy"?
Share this article. It could prevent their cancer.
Medical Disclaimer
This article is provided strictly for educational, informational, and awareness purposes only. It is not intended to be, and should not be construed as, professional medical advice, diagnosis, treatment, or a substitute for consultation with qualified healthcare professionals.
No Doctor-Patient Relationship
The information presented in this article does not establish a doctor-patient relationship between the reader and the author, publisher, or any affiliated entities. No medical decisions should be made based solely on the content of this article.
Consult Qualified Medical Professionals
If you are experiencing any symptoms mentioned in this article, have been diagnosed with cancer, or have concerns about cancer risk, seek immediate consultation with qualified oncologists, physicians, or appropriate medical specialists. For medical emergencies, contact emergency services immediately.
Individual Medical Situations Vary
Every person's medical condition, health history, risk factors, cancer type, and circumstances are unique. Diagnostic tests, treatment options, and medical recommendations must be tailored to individual patients through direct consultation with licensed healthcare providers who have access to complete medical histories and can perform proper clinical evaluations.
Not a Recommendation for Specific Tests or Treatments
References to biopsies, imaging studies (CT scans, PET scans, MRI), blood tests, tumor markers, chemotherapy, radiation therapy, immunotherapy, targeted therapy, surgery, or any other diagnostic procedures and treatments in this article are for informational purposes only and do not constitute recommendations that you should or should not undergo these tests or treatments. All decisions regarding medical testing, diagnosis, and treatment should be made in consultation with qualified healthcare professionals based on your specific medical situation.
No Guarantee of Accuracy or Completeness
While efforts have been made to provide accurate information, medical knowledge continuously evolves, particularly in the rapidly advancing field of oncology. The information in this article may not reflect the most current research, clinical guidelines, treatment protocols, or medical practices. The author and publisher make no representations or warranties regarding the accuracy, completeness, or timeliness of the content.
Do Not Disregard or Delay Professional Medical Advice
Never disregard, avoid, or delay obtaining professional medical advice from qualified healthcare providers because of something you have read in this article. If you have questions or concerns about information presented here, discuss them with your personal physician or oncologist. Early detection and prompt treatment significantly improve cancer outcomes.
Third-Party Resources and Links
Any references to third-party medical services, clinics, doctors, cancer centers, or external websites are provided for informational purposes only and do not constitute endorsements. The author and publisher are not responsible for the content, services, or practices of any third-party entities.
Limitation of Liability
To the fullest extent permitted by law, the author, publisher, and affiliated entities disclaim all liability for any direct, indirect, incidental, consequential, or punitive damages arising from the use of, or reliance on, information contained in this article. This includes, but is not limited to, medical complications, treatment decisions, financial losses, or any other adverse outcomes.
Geographic and Regulatory Considerations
Medical regulations, standards of care, insurance coverage, availability of diagnostic tests, treatment protocols, and access to cancer therapies vary by country, region, and healthcare system. Information regarding procedures and medical practices may not be applicable to all geographic locations or healthcare settings.
Clinical Trials and Experimental Treatments
Any references to clinical trials, experimental treatments, or investigational therapies are for informational purposes only. Participation in clinical trials should only be considered after thorough discussion with your oncology team and understanding of all risks and benefits.
Your Responsibility
You acknowledge that you are solely responsible for your own health decisions and that you will consult with appropriate licensed healthcare professionals before making any medical decisions or undergoing any diagnostic tests or treatments.
Acknowledgment
By reading and using the information in this article, you acknowledge that you have read, understood, and agreed to this disclaimer in its entirety. You further acknowledge that this article has been created with the assistance of artificial intelligence. While every effort has been made to ensure accuracy, AI-generated content may occasionally contain errors, omissions, or inaccuracies. The information presented here is intended solely for educational and informational purposes and should not be relied upon as a substitute for professional medical advice. Readers are strongly encouraged to consult qualified healthcare professionals, refer to peer-reviewed medical literature, and cross-reference information from established clinical sources before making any health-related decisions.
Last Updated: 5th February 2026
What's Your Reaction?
 Like
0
Like
0
 Dislike
0
Dislike
0
 Love
0
Love
0
 Funny
0
Funny
0
 Angry
0
Angry
0
 Sad
0
Sad
0
 Wow
0
Wow
0